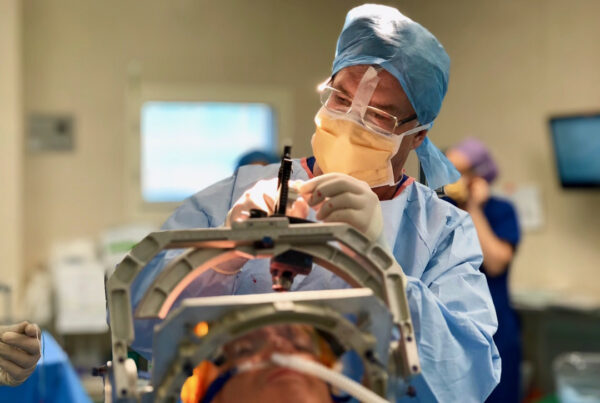
Deep Brain Stimulation (DBS) is a key modern neurological technique.
It uses neurochip technology. Its goal is to enhance electrical connections within targeted brain areas. This aims to alleviate severe neurological disorder symptoms.
In advanced medicine, this technique is one of the most complex. It is also one of the most interesting neurological procedures.
This revolutionary technique is somewhat like a “pacemaker for the brain.” It has become an important treatment option. It helps many intractable neurological conditions.
This operation is performed in advanced centers. An example is Liva Hospital in Istanbul. It’s an advanced treatment option. It’s used when traditional treatments like medication or physical therapy fail.
Indications for Deep Brain Stimulation
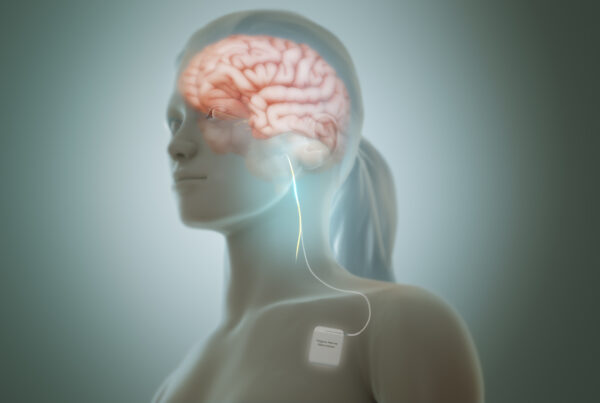
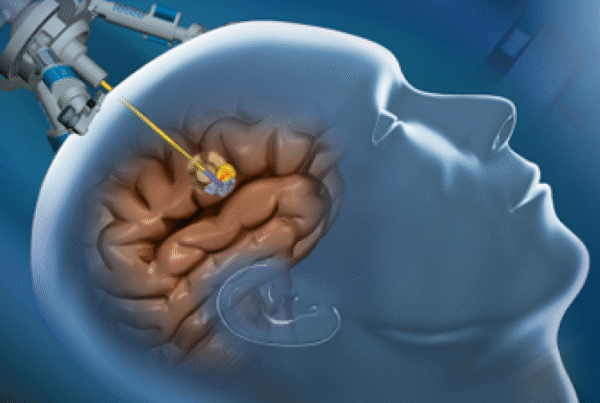
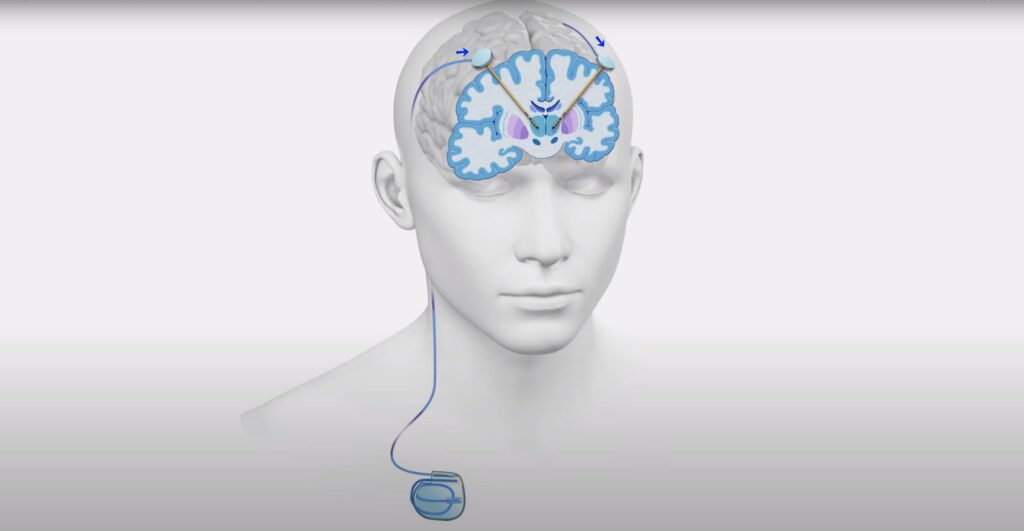
Deep Brain Stimulation (DBS) is a surgical procedure. Electrical electrodes are implanted in specific brain areas.
These electrodes connect to a device. It’s like a pacemaker. It’s implanted under the chest skin. It sends electrical impulses. These regulate abnormal brain activity.
Movement Disorders
DBS is widely used to treat Parkinson’s disease. This is especially true for drug-resistant symptoms.
These include tremor, slowness of movement, and muscle rigidity. Studies show the technique reduces the need for Levodopa.
It can be by over 50% in some patients. It helps improve movement and relieve stiffness.
Parkinson’s Disease
Parkinson’s disease is the main indicator for DBS. Studies show DBS can improve these symptoms. It can be by up to 70-80% in carefully selected cases.
Patients typically suffer from tremors unresponsive to medication. They also have severe muscle rigidity and slow movement.
Essential Tremor and Postural Dystonia
Essential tremor is a common disorder. It can be controlled with stimulation of the subthalamic nucleus.
Or other brain structures. The technique helps significantly reduce tremor. It improves quality of life.
Dystonia
DBS can help relieve muscle spasms for dystonia patients. However, the failure rate for wire breakage or displacement is higher. This is compared to other disorders.
Resistant Epilepsy
Deep brain stimulation is used to treat epilepsy. This is when it doesn’t respond to medication.
DBS has been shown to reduce seizure frequency. This is for some patients who have undergone this traditional treatment.
Neuropsychiatric Disorders
Experimental treatment by stimulating areas like the hippocampus is effective. So is stimulating the temporal cortex.
This is in some cases of obsessive-compulsive disorder. It also helps with treatment-resistant depression.
Clinical cases have shown promising results. However, this treatment approach hasn’t been widely adopted yet.
How is the Procedure Performed?
- Planning Phase: MRI or CT scans are performed. They precisely identify brain targets. An example is the subthalamic nucleus.
- Surgical Implantation: The electrode is inserted through small holes in the skull. Then it connects to a small “pulse generator.” This is implanted under the skin near the collarbone.
- Programming and Follow-up: The electrical signal is activated after a recovery period. It is precisely adjusted. This depends on the patient’s motor or behavioral symptom response.
Early Surgical Complications
Brain Hemorrhage
Internal bleeding may occur. Its incidence rate is usually low. But it can cause a stroke or permanent neurological deficit.
Infection
This includes infections at the electrode entry site. Or around the pacemaker device. This accounts for about 5% of reported cases. Some cases may require temporary device removal.
Incorrect Lead Placement
This can lead to reduced stimulation effectiveness. Or it can cause side effects. Sometimes, re-surgery is needed to correct the position.
Psychological Effects (Depression, Mania, Suicidal Ideation)
This is especially true when stimulating the subthalamic nucleus.
Some patients may experience depression or emotional blunting. This happens after the treatment option. Continuous psychological follow-up is recommended.
Cognitive and Memory Impairment
This includes difficulty speaking. Or slowness in cognitive performance.
This is especially due to systemic interference. Or frontal cortex stimulation during the procedure.
Temporary Seizures or Spasms
These may occur during implantation or initial device adjustment. They may resolve with readjustment of technical parameters.
Device-Related Risks (Hardware-Related)
- Local Infection: This is more common. It requires antibiotic treatment or device removal.
- Lead Fracture or Migration: The incidence is higher in dystonia patients. It sometimes requires surgical repair.

Liva Hospital’s Experience in Turkey
Liva Hospital uses this technique. We follow precise protocols. These include pre-imaging planning.
Also, customized programming is done for each case. This enables effective results. It also minimizes side effects.
Liva Hospital provides comprehensive infrastructure. This includes:
- A multidisciplinary surgical team. They evaluate patients and plan targets.
- The latest neurostimulation systems. Also, post-surgery follow-up.
- Updated protocols. These adjust stimulation levels. They also reduce psychological and cognitive side effects.
The hospital combines global technical expertise. It also provides precise personal follow-up. This enhances success rates.
Conclusion
Deep Brain Stimulation is a prominent example of medical progress. It can significantly transform the lives of patients. This is true for those with chronic neurological diseases.
Deep Brain Stimulation remains one of the most complex treatments. It is also one of the most exciting in neuro-medicine.
While this procedure carries undeniable risks, its potential benefits for certain patients can be remarkable.
With continuous technological advancement and our understanding of the brain, the applications of this technique are expected to expand in the future.
However, the procedure is not without challenges. These are surgical, psychological, cognitive, and technical.
This necessitates careful patient selection. Also, in-depth evaluation and comprehensive long-term follow-up are needed. In this context, specialized centers like Liva Hospital are icons of integrated care. This makes the procedure safer and more effective.
Frequently Asked Questions (FAQ)
What conditions are recommended for DBS?
It’s usually recommended for Parkinson’s patients whose symptoms don’t respond to medication. Also for essential tremor, dystonia, resistant epilepsy, and others depending on the case.
What are the most prominent surgical complications?
Brain hemorrhage, infection, misplaced leads, and potential neurological seizures.
Does deep stimulation cause psychological changes?
Depression, hyperactivity, or even suicidal thoughts may appear in some. Especially without psychological follow-up.
How long does the device’s effectiveness last?
Batteries usually work for 3 to 5 years. Then they need a replacement.
Are all patients eligible?
A precise evaluation of general health, cognition, and life expectations is required before implantation.
Why is Liva Hospital an excellent choice?
It provides an accurate evaluation. It has an internationally qualified team. It uses modern equipment. It also offers comprehensive post-operative follow-up.